Canberra Hospital is rolling out specialised computers to help staff take blood samples, after an audit found long-standing problems pathology collection.
Subscribe now for unlimited access.
or signup to continue reading
An internal audit of pathology sample management last September found a consistently high number of incidents of "non-compliance with specimen labelling and patient identification" in the emergency department and ward 14B over the past two years.
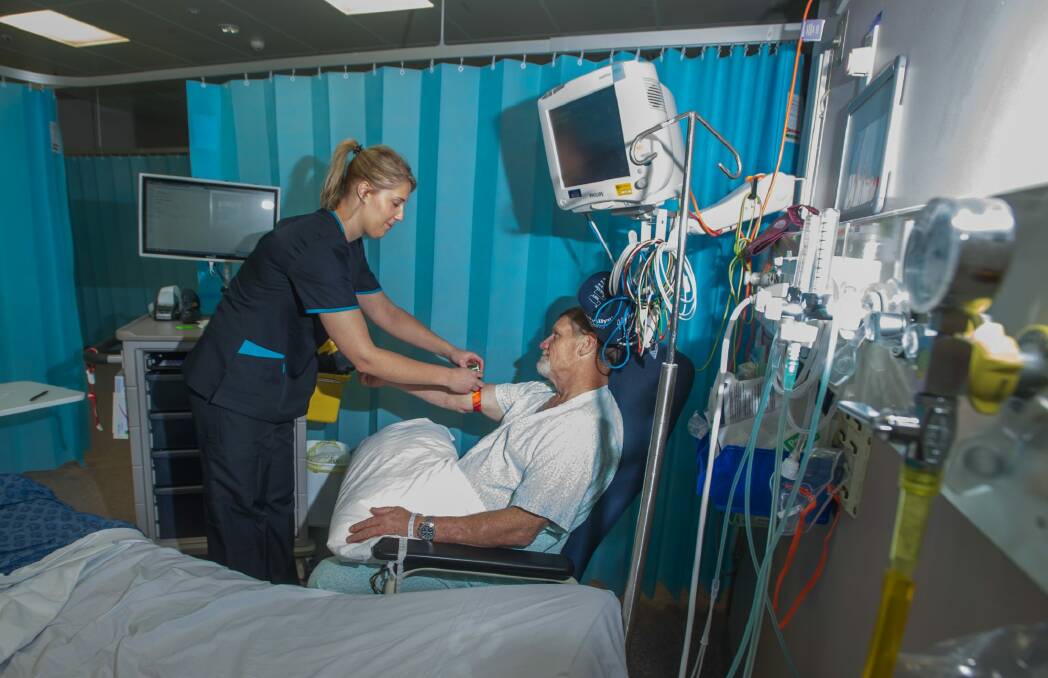
Such errors can lead to people getting the wrong treatments and in the most dire of cases, receiving the wrong blood in transfusions.
The audit, obtained under Freedom of Information laws, also revealed that there had been "no declining trends" in the number of incidents in recent years despite new policies and procedures being put in place to reduce such errors.
In response, hospital management agreed to review practices in the emergency department to ensure staff followed the ":positive patient identification requirements for the collection and labelling of blood samples", as part of a wider response.
The errors mainly stemmed from staff, under constant pressure in busy wards, failing to positively identify patients during blood sample collections and ensure blood samples were correctly labelled for the pathology unit to do the right tests.
While ACT Health's director of the blood counts program, Dr Philip Crispin, said patients being given the wrong blood in a transfusion could be life-threatening, he called such events a "never ever" situation, and there had only been two such cases in his 10 years at Canberra Hospital.
He said the audit had been undertaken as part of a wider national effort by hospitals to ensure they were meeting the National Standard for Blood and Blood Products that became mandatory in 2013, leading to a more rigorous focus on risks.
"It's an ongoing situation we've been trying to address for quite a while, but it was really the national standards that gave us all a focus on it, particularly for transfusions, but it's really the same story across the country," Dr Crispin said.
"We took a bigger focus on risk prevention and we realised patient identification was a big issue."
While the hospital already has about 100 COWs for different purposes on different wards, management is now looking to standardise them down to two models only, to cover blood testing and collection, medication management and several other purposes.
The plan, an ACT Health spokeswoman said, was to have some 300 COWs operating across the hospital by June 2018 to help doctors and nurses ensure correct procedures are in place and help rule out any errors.
Dr Crispin said those machines would also be connected to a central IT "Positive Patient Identification" (PPID) system which would, by scanning various barcodes, ensure only the right labels were put on the right blood samples for the right person at the bedside.
He said that could also reduce the need for multiple samples for each patient to be collected, and cut down on unnecessary blood tests as well, as the PPID system would connect to individual patient records as well.
"One of the main problems we have in this space is it's human-based and that can lead to human error," Dr Crispin said.
"With the computer systems once it's rolled out, we can reach levels of risk prevention we never could have before, and we've already been trying all these things and have had some success already."

